Patient financial services manager
Revenue cycle director
Financial counselor
Chief financial officer
Community benefit coordinator
Patient access supervisor

This process is used when patients request financial assistance for healthcare services they cannot afford. It is triggered when patients indicate inability to pay during registration, when self-pay accounts reach certain aging thresholds, when patients apply for financial assistance programs, when emergency care is provided to uninsured patients, or when existing payment arrangements become unmanageable. The process becomes essential when nonprofit hospitals must demonstrate community benefit, when regulatory requirements mandate financial assistance policies, when large balances require write-off decisions, or when equitable treatment of financially distressed patients must be documented. Ideal for nonprofit health systems with community benefit obligations, hospital revenue cycle operations, federally qualified health centers, and any healthcare provider offering financial assistance programs.
This process typically involves patients who apply for assistance and provide financial documentation, financial counselors who guide patients through the application process and gather required information, patient financial services specialists who verify documentation and calculate eligibility, revenue cycle managers who review applications against policy criteria, approval committees who authorize assistance for complex cases or large amounts, and finance leadership who oversee charity care budgets and policy compliance. Social workers may participate when patients need additional support services.
Equitable assistance determination with consistent policy application ensuring similar patients receive similar treatment. Documented eligibility verification supporting audit and regulatory compliance requirements. Timely patient communication so patients understand their financial responsibility or assistance award promptly. Accurate community benefit reporting when charity care is properly classified and valued. Reduced collection activity on accounts appropriately identified for charity care rather than aggressive collection.
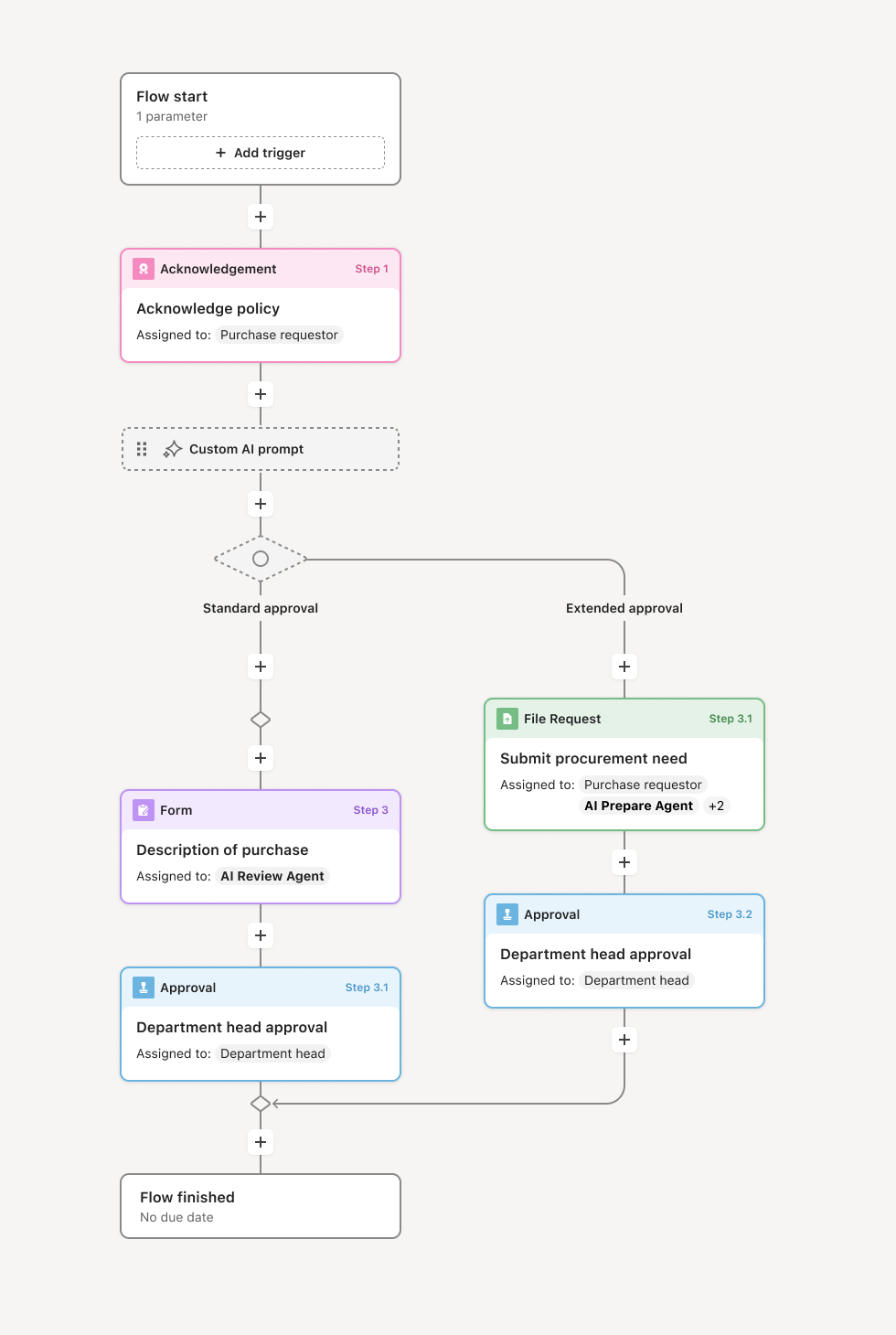
Your version of this process may vary based on roles, systems, data, and approval paths. Moxo's flow builder can be configured with AI agents, conditional branching, dynamic data references, and sophisticated logic to match how your organization runs this workflow. The steps below illustrate one example.
Application initiation and patient outreach
The process begins when a patient is identified as a potential charity care candidate. This may occur during registration when a patient discloses financial hardship, through proactive screening of self-pay accounts, or when patients directly request assistance. A financial counselor reaches out to explain available programs, provide application materials, and guide the patient through documentation requirements. The application collects household size, income sources, employment status, assets, and other financial information needed to assess eligibility. An AI agent can assist by pre-screening based on available data, identifying patients likely to qualify, and preparing applications with known information.
Documentation collection and verification
The patient provides documentation supporting their financial situation. This typically includes proof of income such as pay stubs or tax returns, proof of household composition, bank statements, and documentation of other financial obligations or hardships. Financial counselors work with patients to obtain complete documentation, explaining what is needed and following up on missing items. Verification may include income validation against reported amounts, confirmation of household size, and assessment of asset levels. If documentation is incomplete, the patient is contacted to provide additional information before the application can proceed.
Eligibility calculation and determination
Patient financial services calculates eligibility based on the organization's charity care policy. This typically involves comparing household income to federal poverty guidelines, assessing whether income falls within defined percentage thresholds for full or partial assistance, considering assets that may affect eligibility, and applying any policy exceptions for extraordinary circumstances. The calculation determines whether the patient qualifies for full charity care, partial discount, payment plan, or denial. For straightforward cases meeting clear criteria, eligibility may be determined directly; complex cases advance to committee review.
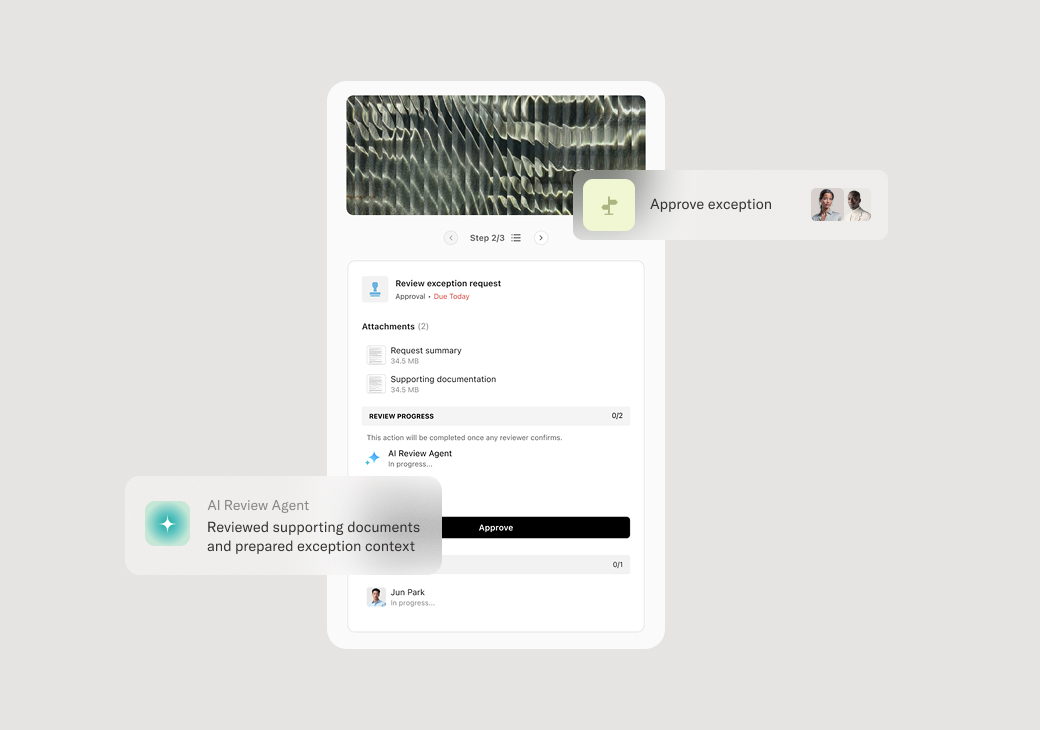
Review and approval authorization
Applications are routed to appropriate approvers based on assistance amount and complexity. Standard applications within policy guidelines may be approved by financial services managers. Large write-offs, policy exceptions, or cases with unusual circumstances may require review by a charity care committee or finance leadership. Approvers review the application, supporting documentation, and eligibility calculation before rendering a decision. If additional information is needed, the application is returned for supplementation. Approval specifies the assistance amount or percentage and any conditions.
Patient notification and account adjustment
Once approved, the patient is notified of the assistance decision. Notification includes the approved discount or write-off amount, any remaining patient responsibility, and next steps such as payment plan options for remaining balances. The patient account is adjusted to reflect approved charity care, and the write-off is recorded with appropriate classification for community benefit reporting. The workflow maintains the complete application record including documentation, eligibility calculation, approval chain, and patient communication for compliance and audit purposes.
This process commonly relies on inputs such as patient financial applications, income documentation, federal poverty guideline tables, organizational charity care policies, patient account balances, and insurance coverage information. It may be triggered by patient requests, self-pay account aging, proactive screening programs, or social work referrals. Common systems that integrate with this workflow include hospital information systems like Epic or Cerner, revenue cycle management platforms, patient portal systems for application submission, document management systems for supporting paperwork, and financial reporting systems for community benefit tracking.
Key decision points include determining whether documentation is sufficient to assess eligibility, whether income and assets fall within policy thresholds for assistance, whether full or partial assistance is appropriate, whether policy exceptions are warranted for extraordinary circumstances, and whether approval authority resides with staff or requires committee review. Each decision point may trigger requests for additional documentation, escalation to committee review, adjustment of assistance levels, or denial with explanation and appeal options.
Incomplete applications where missing documentation delays determination and leaves patients uncertain about their responsibility. Inconsistent eligibility decisions when similar patients receive different outcomes due to varied policy interpretation. Delayed processing where applications languish while accounts are sent to collections inappropriately. Inadequate patient communication when patients are not informed of programs or do not understand application requirements. Documentation retention gaps when records are insufficient to support audit or regulatory review of charity care decisions.
Orchestrates the complete assistance cycle from patient outreach through documentation collection, eligibility determination, and approval in a single coordinated flow.
Engages patients securely providing a private channel for sensitive financial information submission and counselor communication.
AI agents screen eligibility and validate documentation pre-calculating likely qualification and flagging incomplete applications before review.
Connects to hospital and revenue cycle systems so patient account data flows in automatically and approved adjustments can update billing records.
Routes by assistance amount and complexity so routine approvals proceed quickly while large write-offs and exceptions receive appropriate committee review.
Maintains complete eligibility records with timestamps, documentation, calculations, and approval chains for compliance, community benefit reporting, and audit.