Claims manager
Senior claims adjuster
Medical review specialist
Fraud investigator
Finance director
Compliance officer
Legal counsel
External medical examiner

Claims payment approval is triggered when initial claim assessment is complete and payment recommendation requires formal authorization. This process becomes critical when claim amounts exceed adjuster authority limits, when medical complexity requires specialist review, or when fraud indicators demand investigation. It's essential for insurance carriers, self-insured employers, third-party administrators, and government benefit programs managing high-value or complex claims.
Claims managers coordinate the approval workflow and ensure proper routing based on claim characteristics. Senior adjusters provide detailed assessments and payment recommendations. Medical reviewers evaluate treatment necessity and cost reasonableness. Finance teams verify payment authority and process disbursements once approved.
Faster payment authorization as claims move through appropriate review levels without manual routing delays. Reduced payment errors from systematic validation of coverage, limits, and calculation accuracy before authorization. Consistent application of approval thresholds ensuring proper authority levels review high-value or complex claims. Earlier fraud detection through coordinated review of suspicious patterns and documentation gaps. Improved regulatory compliance with documented approval chains and timely payment processing meeting statutory requirements.
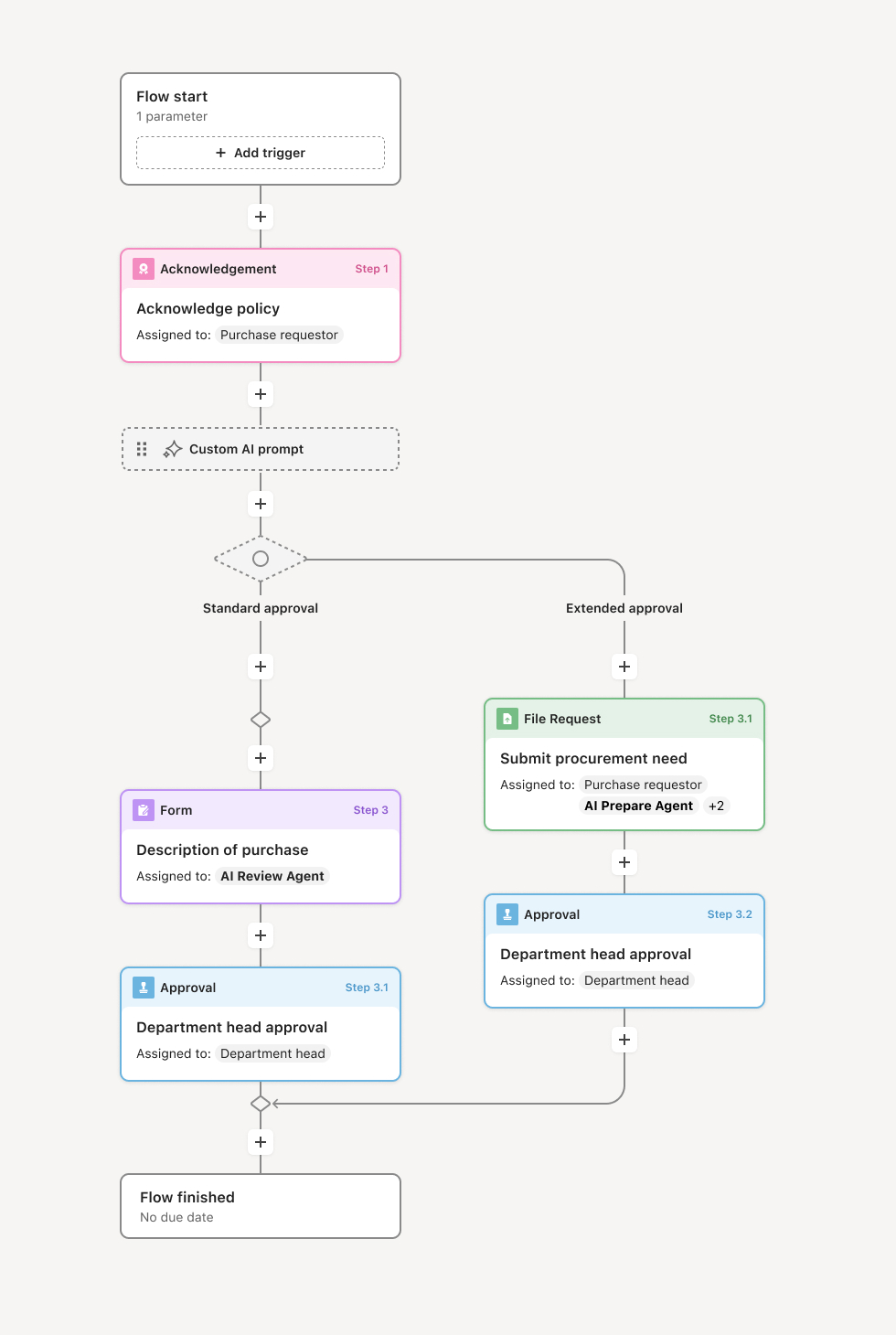
Your version of this process may vary based on roles, systems, data, and approval paths. Moxo's flow builder can be configured with AI agents, conditional branching, dynamic data references, and sophisticated logic to match how your organization runs this workflow. The steps below illustrate one example.
Initial Review and Routing
The process begins when a claim assessment reaches payment recommendation stage. AI agents analyze claim characteristics including amount, complexity, and risk indicators to determine appropriate review path. Claims exceeding standard adjuster authority are automatically routed to senior review, while those with medical complexity trigger specialist evaluation. The system validates that all required documentation is present before proceeding.
Authority Level Determination
Based on payment amount and claim type, the workflow routes to appropriate approval authority. Standard claims within limits proceed to adjuster approval, while high-value claims escalate to claims managers or directors. If fraud indicators are present, the claim branches to investigation workflow before returning to payment approval. AI agents prepare approval packages with claim summary, payment calculation, and supporting documentation.
Specialist Review and Validation
For claims requiring medical or technical review, specialists evaluate treatment necessity, cost reasonableness, and policy coverage. External medical examiners may be engaged for complex cases. AI agents flag inconsistencies between medical records and treatment codes, highlighting areas requiring human judgment. Reviewers can request additional documentation or recommend payment adjustments.
Approval Decision and Documentation
Authorized approvers review the complete claim package and make final payment decisions. If approved, the workflow advances to payment processing with documented rationale. If denied or adjusted, detailed explanations are captured for claimant communication. AI agents ensure all regulatory timing requirements are tracked and escalate approaching deadlines.
Payment Processing and Communication
Approved payments are transmitted to finance systems for disbursement processing. Claimants receive automated notification of approval decisions with payment details and timing. For denied or adjusted claims, formal letters are generated with appeal rights and procedures. The complete approval record is maintained for audit and regulatory reporting.
This process typically pulls claim data from core insurance systems (Guidewire ClaimCenter, Duck Creek Claims, FINEOS), medical records from provider networks, and fraud scoring from analytics platforms (SAS Fraud Framework, FICO Falcon). It is triggered when claim assessment reaches payment recommendation status, when amounts exceed adjuster authority, or when risk scores indicate review requirements. Key inputs include claim files, medical documentation, policy terms, payment calculations, and regulatory compliance checklists.
Key decision points include determining whether claim amounts require escalated approval authority, whether medical complexity warrants specialist review, and whether fraud indicators demand investigation before payment. Additional decisions involve payment amount adjustments based on coverage limits, coordination of benefits calculations, and timing of payment to meet regulatory requirements.
Approval delays from unclear authority levels causing claims to stall while routing decisions are made manually. Incomplete documentation packages reaching approvers without required medical records or policy verification. Missed regulatory deadlines from lack of visibility into approval timing requirements. Inconsistent fraud screening allowing suspicious claims to bypass proper investigation protocols. Payment calculation errors from manual coordination of benefits or deductible applications not caught before approval.
AI agents analyze claim characteristics and automatically route to appropriate approval authority based on amount, complexity, and risk indicators.
Conditional branching ensures proper review paths with medical claims triggering specialist evaluation and high-value claims escalating to senior management.
Integrated validation checks confirm policy coverage, calculate payment amounts, and verify regulatory compliance before approval packages reach decision-makers.
Real-time escalation triggers surface approaching regulatory deadlines and stalled approvals requiring immediate attention.
Parallel coordination allows fraud investigation and medical review to proceed simultaneously when both are required.
External specialist participation enables medical examiners and legal counsel to complete reviews directly within the approval workflow.